Emergency Dentistry
Root Canals Aren't All the Same — Here's What Actually Determines the Outcome
Two root canals on paper can look identical — same tooth, same procedure code — and have completely different outcomes. The variables that actually matter are tooth complexity, the imaging and disinfection technology used, and whether saving that tooth is even the right call clinically. This article breaks down all three.
Why Root Canals Vary So Much From Patient to Patient
Most patients assume a root canal is a root canal. It isn't. The procedure that gets coded the same way at two different practices can involve very different levels of precision — and the outcome differences are real.
A standard root canal on a front tooth, performed by a general dentist using 2D X-rays, sits at the simpler end of the spectrum. A molar root canal performed by an endodontic specialist using CBCT (cone-beam computed tomography) 3D imaging sits at the complex end — and for good reason. CBCT scans reveal canal anatomy that flat X-rays miss entirely. Molars commonly have four or five canals; miss one, and the infection returns. A procedure that looked successful at the time can fail within a year or two and lead to retreatment or extraction.
Some practices also use advanced cleaning systems like GentleWave, which uses multispectral acoustic energy to disinfect canal systems more thoroughly than traditional hand filing. These technologies meaningfully reduce retreatment rates. The tradeoff in upfront complexity often translates into a "one-and-done" result rather than the first step in a longer sequence of repeated work.
For Long Beach-area patients, the bigger variable — by far — is what kind of root canal you're getting, and almost always a tooth crown follows to protect the treated tooth.
WebMD's root canal overview confirms the procedure itself — removing infected pulp, cleaning, sealing — is standard. What varies is the precision of execution.
When Saving the Tooth Isn't the Right Call
This is the conversation most patients never hear, and it matters more than any other factor.
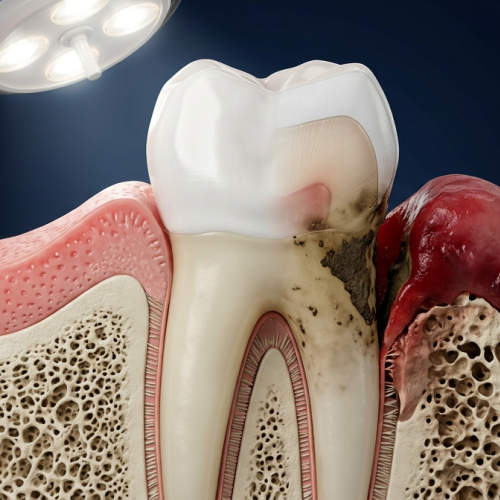
Not every tooth should be saved with a root canal. I look for specific clinical markers before recommending endodontic root canal treatment. A vertical root fracture, for instance, is a near-absolute contraindication — the tooth will fail regardless of how well the root canal is performed. Internal resorption, severe bone loss around the root, or a tooth with insufficient remaining structure to hold a crown all fall into what we call a "guarded prognosis."
A tooth with a guarded prognosis that fails within a year or two leaves the patient worse off than if the tooth had been replaced from the start. Research published in PMC comparing root canal treatment to extraction found that while root canal treatment preserved quality of life better short-term, the potential need for future replacement significantly affected long-term outcomes. The decision isn't simply "save the tooth at all costs" — it's about giving the tooth an honest read.
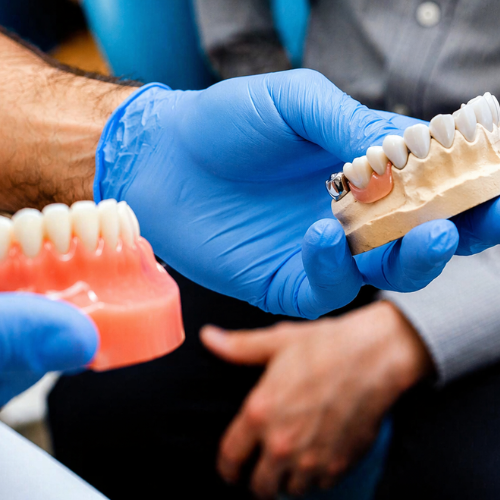
The American Association of Endodontists is clear that saving a natural tooth should always be the first priority — but they also acknowledge that when a tooth cannot be saved, dental implants are the appropriate next step. My job is to give you an honest read on which category your tooth falls into before you commit to either path.
Why I Might Tell You "No" to an Implant
Patients are sometimes surprised when I recommend against an implant. The reasons go beyond obvious health conditions.
The most commonly overlooked factor is medication. Bisphosphonates — drugs taken for osteoporosis like alendronate (Fosamax) — are a well-documented contraindication. They suppress bone turnover, which means the jawbone can't remodel properly around a titanium post. In severe cases, patients on intravenous bisphosphonates face a risk of osteonecrosis of the jaw. Mayo Clinic's implant surgery guide lists this specifically among conditions that affect bone healing.
Less known: SSRIs (antidepressants like sertraline and fluoxetine) appear to interfere with bone metabolism and have been associated with increased implant failure rates in emerging research. A patient can be otherwise healthy — no diabetes, no smoking, no gum disease — and still face elevated implant failure risk because of a medication their physician prescribed for an entirely different condition.
Other relative contraindications include active smoking, uncontrolled diabetes, autoimmune conditions affecting healing, and prior radiation to the head and neck. Healthline's implant safety overview covers several of these, though the medication angle is frequently underemphasized in patient-facing resources.
When I decline to recommend an implant, I'm not dismissing the option — I'm protecting you from a procedure that has a meaningful chance of failing and leaving you worse off than before.
What to Ask Before You Decide
The decision almost always comes down to three things: what imaging and technology your dentist is actually using (which affects long-term success), whether the tooth in question is structurally worth saving at all, and — if an implant is on the table — whether your medical history and medications support a successful outcome.
If your dentist is recommending a root canal, ask specifically about the imaging technology being used and whether the tooth has a favorable or guarded prognosis. If an implant is being considered, ask whether any medications you take could affect osseointegration. These aren't difficult questions — any dentist should welcome them.
Clarity about the procedure matters. So does making sure the treatment being recommended is the right one for your specific clinical situation.
Talk to Our Long Beach Team About Your Options
At Long Beach Family Dentist, we handle both root canal therapy and implant consultations under one roof — with sedation options for patients who are anxious about either procedure. If you've been told you need a root canal, or if you're weighing whether to save or replace a tooth, we'll give you a straight answer backed by a thorough cleaning and exam and clinical evaluation. Serving patients throughout the Long Beach metro area.
Medical disclaimer: This article is for informational purposes only and does not constitute professional dental or medical advice. Treatment decisions should be made in consultation with a licensed dental provider based on your individual clinical situation.