Emergency Dentistry
When Is It Too Late to Treat Periodontitis? What Every Long Beach Patient Needs to Know
Periodontitis is almost never completely "too late" to treat, but there are real thresholds where your options shrink dramatically — and the costs multiply. Understanding where those thresholds are can save your teeth, your bone, and thousands of dollars.
The Real "Point of No Return" Isn't Losing a Tooth — It's Losing the Bone Beneath It
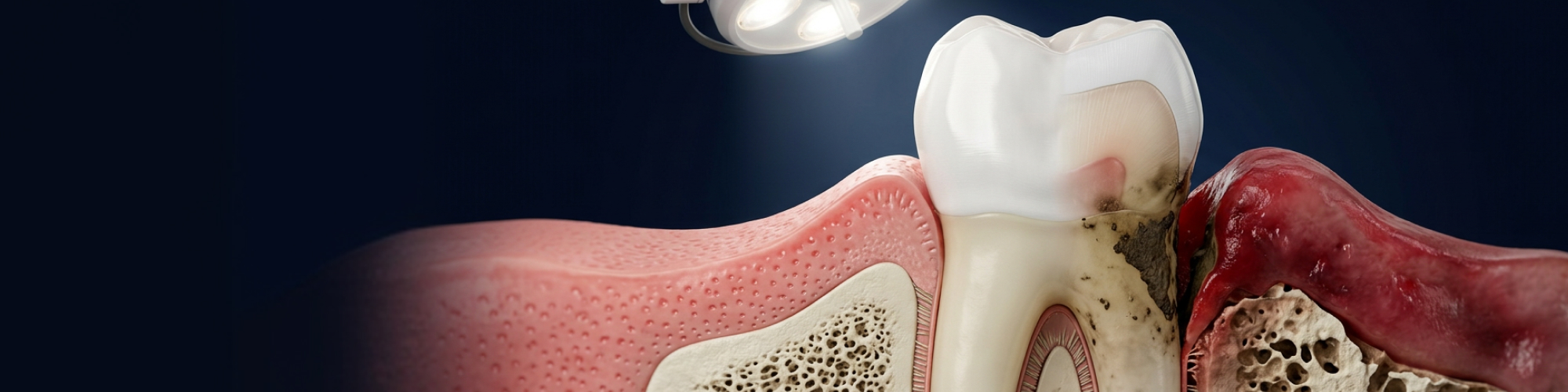
Most patients come to me worried about a loose tooth. For Long Beach-area patients, I have to explain that the tooth itself is often the last thing to go. The bone that anchors it starts disappearing months or years earlier, silently, without pain.
According to the Mayo Clinic, periodontitis damages the soft tissue and destroys the bone supporting your teeth — and that destruction is largely irreversible once it progresses far enough.
Here’s what that means in practical terms: a standard dental implant requires a sufficient amount of bone height and width to seat properly. Advanced periodontitis doesn’t just threaten your teeth—it progressively consumes the alveolar ridge itself. When patients wait too long, the issue often isn’t replacing the lost tooth. It’s that there’s no longer enough bone to support an implant.
That shift changes everything. Instead of moving directly to implant placement, the focus turns to rebuilding what’s been lost. That can involve bone grafting procedures and, in the upper jaw, potentially a sinus lift—steps that add time, complexity, and recovery to what could have been a more straightforward process. By contrast, addressing gum disease at a moderate stage with scaling and root planing is typically far less involved. Delaying treatment until significant bone loss has occurred can turn a relatively contained problem into a much more extensive reconstruction. The “too late” threshold that actually matters isn’t tooth loss. It’s bone volume loss. The ADA notes that roughly 42% of dentate U.S. adults age 30 and older have some form of periodontitis—many of them unaware, because the disease often progresses without pain until significant damage is already done.
Why Your Toothbrush Physically Cannot Fix This After a Certain Point
One of the most common things I hear: "I've been brushing more carefully — shouldn't that help?" The answer depends entirely on how deep your gum pockets are, and here's why.
A toothbrush bristle reaches about 2–3mm below the gumline. Floss reaches roughly the same depth. In a healthy mouth, pockets measure 1–3mm — well within range of home care.
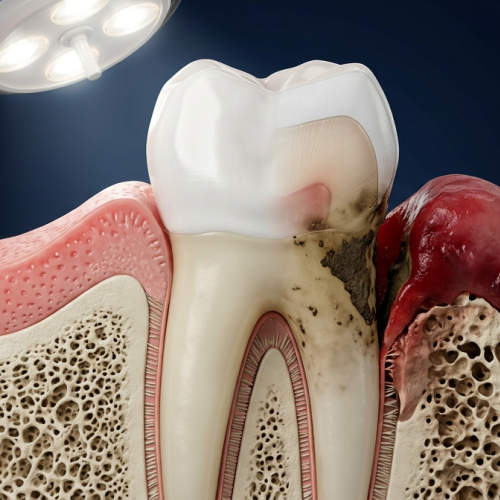
Once pockets reach 4–5mm, you're in early-to-moderate periodontitis territory. Home care becomes insufficient, but professional deep cleaning (scaling and root planing) is highly effective. At 6mm and beyond — what we classify as advanced or Stage III/IV periodontitis — the bacteria colonizing the base of those pockets are physically unreachable by any tool you own. The American Academy of Periodontology explains that scaling and root planing involves professional instrumentation deep beneath the gumline to remove bacterial toxins that home care simply cannot access.
This isn't about effort or technique. It's geometry. The pocket is deeper than your tools can reach. The idea that you can "cure" 6mm+ pockets with oil pulling or a water flosser is anatomically impossible. What you can do is stop the progression from getting worse at home — but you cannot reverse what's already there without professional intervention.
At Stage III and IV, surgical options like flap surgery become necessary precisely because the anatomy has changed too dramatically for non-surgical access. In some cases, severely compromised teeth may ultimately require tooth extraction when the supporting structures can no longer be salvaged.
The Open Wound You Don't Know You Have
People often tell me they'll "deal with it later" when I mention gum disease. I understand — it doesn't hurt, and life is busy. But I want you to consider something.
If you have Stage III or IV periodontitis, the inflamed, ulcerated tissue lining your gum pockets adds up to a surface area roughly the size of the palm of your hand. That's not a metaphor for severity — that's a literal approximation of infected, open tissue inside your mouth, in constant contact with your bloodstream.
Would you leave a palm-sized infected wound on your arm untreated for two years?
That chronic infection drives up systemic inflammation markers, including C-Reactive Protein (CRP), which is directly linked to cardiovascular risk. Harvard Health reports that people with gum disease have two to three times the risk of serious cardiovascular events. Research has also linked the primary periodontal pathogen Porphyromonas gingivalis to Alzheimer's disease risk and adverse pregnancy outcomes.
Research published in PMC confirms that periodontitis involves complex interactions between bacterial pathogens and the host immune response — meaning your own body's inflammatory reaction is driving much of the tissue destruction, and that same inflammation doesn't stay neatly contained to your gums.
This is why treating gum disease isn't cosmetic. It's systemic care.
How to Know Where You Stand Right Now
The honest answer to "how do I know if I have advanced gum disease?" is that you probably can't tell on your own. The disease is largely painless until late stages. Here's what I look for during an exam:
- Pocket depths of 4mm or more — measured with a periodontal probe at multiple sites
- Bleeding on probing — a reliable early inflammation marker
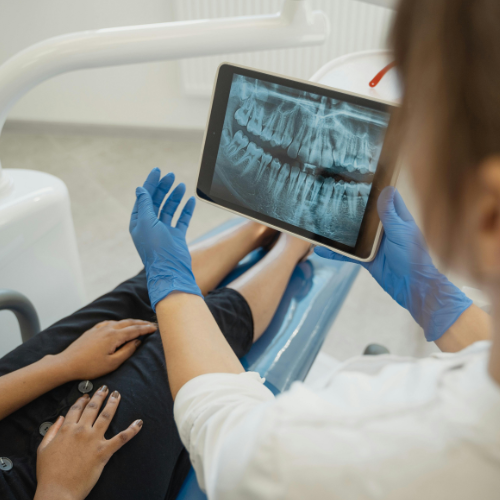
- Radiographic bone loss — visible on X-rays before symptoms appear
- Tooth mobility — a late-stage finding indicating significant bone loss
- Gum recession — pockets that expose root surfaces
The warning signs you can watch for yourself include gums that bleed when brushing, persistent bad breath, teeth that look longer than they used to, or any looseness in teeth. If you're noticing any of these, don't wait. Scheduling a cleaning and exam is the most important first step you can take toward getting an accurate picture of your periodontal health.
The staging system — Stage I through Stage IV — is assigned by your dentist or periodontist based on bone loss percentage, pocket depth, tooth mobility, and complexity of treatment needed. Stage I and II are manageable with non-surgical care. Stage III and IV typically require surgical intervention. None of them are hopeless, but each stage represents a narrowing of your options and a rising cost of treatment. In cases where infection has reached the tooth's root, an endodontic root canal may also be necessary to address damage that has extended beyond the gum tissue.
Ready to Find Out Where You Stand?
If you're in the Long Beach area and have been putting off a gum evaluation, I'd encourage you not to wait longer. At Long Beach Family Dentist, our team performs comprehensive periodontal evaluations and offers the full range of treatment — from non-surgical deep cleaning to advanced surgical care — all under one roof with sedation options for anxious patients. The earlier we catch this, the more we can preserve. Call us to schedule your evaluation today.
Medical disclaimer: This article is for informational purposes only and does not constitute medical or dental advice. Always consult a licensed dental professional for diagnosis and treatment recommendations specific to your condition.