Specialty Dentistry
Understanding Oral Sedation Dentistry: What Long Beach Patients Need to Know
I've been practicing dentistry in Long Beach for years, and honestly, the most common question I hear isn't about procedures—it's about fear. Patients want to know if they'll feel pain, if sedation is safe, and what it's actually like to be sedated during dental work.
Look, I get it. The anxiety around dental visits is real, and it's completely valid. That's why we offer oral sedation dentistry at our practice—it's changed the game for patients who would otherwise avoid necessary treatment. Unlike general anesthesia where you're completely unconscious, oral sedation keeps you in a relaxed state where you can still respond to instructions (which, fair enough, makes it safer for outpatient dental procedures).
Here's the thing: most people have misconceptions about what sedation dentistry actually involves. They picture being knocked out cold or worry about dangerous side effects. But the reality? It's a carefully monitored process that's helped thousands of Long Beach patients finally get the dental care they've been putting off. We'll walk through exactly what happens, what it feels like, and whether you'll experience pain—because you deserve straight answers before making any decisions about your dental health.
Is sedation dentistry dangerous?
Honestly, this is the question that keeps some patients from getting treatment they desperately need. And I understand why—you're putting trust in medications that alter your consciousness. That's not something to take lightly.
But here's the reality: when performed according to current ADA and AAPD guidelines, sedation dentistry is remarkably safe. I'm talking about strict protocols for patient evaluation, dosing limits, continuous monitoring, and trained personnel. The key word there? Guidelines. Not all practices follow them equally (which, I'll admit, is a controversial opinion—but state boards need stricter enforcement).
I had a patient last month who'd avoided the dentist for eight years because of a horror story she'd heard online. Actually, scratch that—it wasn't just online rumors. There have been tragic cases of sedation-related complications. But when you dig into those cases, you find a pattern: guideline non-compliance, inadequate monitoring, or providers exceeding their training level.
At our Long Beach practice, we follow maximum recommended doses to the letter. We continuously monitor your airway, oxygen levels, heart rate, and blood pressure throughout the procedure. And we don't let you leave until you meet specific safety discharge criteria. Bottom line? The risks—respiratory depression, airway obstruction, cardiovascular issues—are preventable with proper protocols.
The different sedation levels carry different risk profiles. Minimal sedation like nitrous oxide? Incredibly low risk with rapid recovery. Moderate oral sedation? Still quite safe when dosed correctly. Deep sedation and general anesthesia? Higher resource requirements and risks, reserved for specific cases.
I'm not 100% sure why some practitioners still take shortcuts with monitoring, but my theory is it's a combination of cost-cutting and overconfidence. Don't let that be your dentist. Ask about their training, monitoring equipment, and emergency protocols before agreeing to sedation.
What does conscious sedation feel like?
This question always makes me smile because patients expect some mystical experience, but the reality is much more... mundane? You're basically really, really relaxed.
Conscious sedation—or moderate sedation as we call it clinically—puts you in a depressed state of consciousness where you can still respond to verbal commands or light touch. You're not knocked out. You maintain your own airway and breathing. But you're calm enough that the dental work doesn't trigger anxiety or discomfort.
Most patients describe it as a dreamlike state, according to Healthline's overview of conscious sedation. Time perception gets wonky—a 90-minute procedure might feel like 15 minutes. You might remember parts of the procedure or none of it at all. And that's perfectly normal. The medications we use (midazolam is the most common oral sedative) affect memory formation, which honestly helps because who wants to remember the sound of a dental drill?
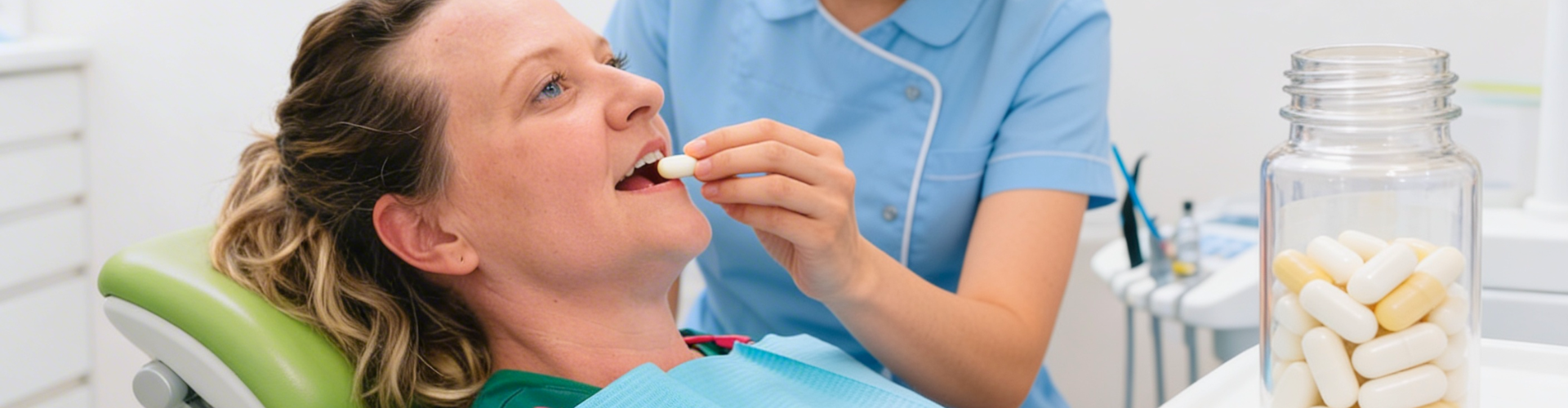
Here's what typically happens: you take the medication about an hour before your appointment. You'll start feeling drowsy and loose-limbed. Some patients get giggly. By the time you're in the chair, you're cooperative but deeply relaxed. We numb the area with local anesthetic (because sedation doesn't block pain—only anxiety and perception), and then we work while you drift in this pleasant, fuzzy state.
Look, it's not like being drunk or high, though some patients make that comparison. It's more like that feeling right before you fall asleep when your thoughts start getting random and your body feels heavy. You won't care what's happening. You might hear us talking or feel pressure, but it won't bother you.
After the procedure, you'll be drowsy for several hours. That's why you need someone to drive you home. Recovery is gradual—you'll feel progressively more alert, though some people report mild headaches or nausea. Not dangerous, just temporarily annoying.
Do you feel pain with oral sedation?
Short answer? Not if we're doing our job right.
But let me clarify something important that confuses a lot of Long Beach patients: oral sedation doesn't block pain. It reduces anxiety and alters your perception and memory of the procedure. Pain control comes from local anesthetics—the injections that numb specific areas of your mouth.
This is where the 2018 ASA guidelines are crystal clear: sedatives must be combined with analgesics (pain blockers) for procedures that would otherwise be painful. We never rely on sedation alone for pain management. That would be ineffective and unethical.
So what does this mean for you during a filling, crown prep, or root canal? We administer the oral sedative to get you relaxed, then we use local anesthetic injections to completely numb the treatment area. You might feel pressure or movement—like pushing or tugging—but actual pain? No. And because you're sedated, even the pressure sensations don't trigger anxiety the way they might otherwise.
I had a patient recently who was terrified of needles. She'd rather have a root canal without anesthetic than get a shot (which, honestly, is wild to me). We used oral sedation first to calm her down, then administered the local anesthetic while she was in that relaxed state. She barely remembered the injection afterward and felt zero pain during the procedure.
Here's the thing: if you do feel pain during the procedure, tell us immediately. Even if you're sedated, you can and should communicate discomfort. We can add more local anesthetic without any problem. And believe me, we want you comfortable—not just for your sake, but because a relaxed patient makes our job infinitely easier.
The combination approach—sedation for anxiety plus local anesthetic for pain—is why oral sedation works so well. You get the best of both worlds: a calm mental state and complete pain control. Recovery involves some lingering drowsiness and maybe slight soreness where we worked, but that's manageable with over-the-counter pain relievers.
Experience Comfortable Dentistry at Long Beach Family Dentist
You shouldn't have to choose between dental health and peace of mind. At Long Beach Family Dentist, we've helped countless anxious patients finally get the treatment they need through safe, monitored oral sedation.
Whether you need a routine filling or extensive restorative work, we'll create a sedation plan tailored to your anxiety level and medical history. Our team follows strict ADA protocols, uses state-of-the-art monitoring equipment, and prioritizes your safety above everything else. And honestly? Seeing patients leave our office saying "that wasn't bad at all" never gets old.
Ready to stop avoiding the dentist? Give us a call to discuss whether oral sedation is right for your next appointment. We'll answer all your questions, explain exactly what to expect, and help you make an informed decision about your care.
Medical Disclaimer: This content is for informational purposes only and does not replace professional medical advice, diagnosis, or treatment. Always consult with a qualified healthcare provider.