Restorative Dentistry
Dentures vs. Dental Implants: What Most Comparisons Don't Tell You
The Palate Factor: Why Dentures Change How Your Food Tastes
This is the detail most patients never hear until after they've committed to a full upper denture. For Long Beach-area patients, understanding these sensory changes is vital. The acrylic base of a conventional upper denture covers your entire hard palate — the roof of your mouth. That coverage does more than feel bulky. Your palate contains thermoreceptors and contributes to how your brain processes flavor and food temperature.
When acrylic sits over that surface, it acts as an insulator. The result? That first sip of morning coffee feels lukewarm. A bowl of soup loses its warmth before it registers. Food can taste muted, flat, or just different than it used to. This isn't psychological — it's a direct consequence of blocking sensory input that your brain expects.
Cleveland Clinic notes that full dentures rest on the gums and rely on the palate for support — which is precisely what creates this coverage problem.
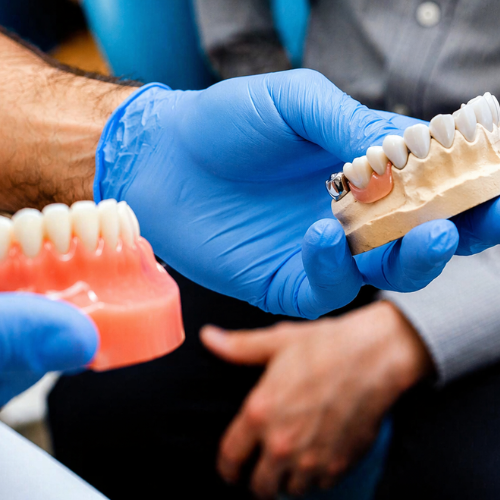
Dental implants — whether single crowns, implant-supported bridges, or fixed full-arch restorations — leave the palate completely uncovered. Your sensory experience at the dinner table stays intact. For patients who love food, who cook, or who simply want eating to remain a pleasure, this distinction matters enormously.
Partial dentures occupy a middle ground. If you're only replacing a few lower teeth, palate coverage isn't an issue. But a partial in the upper arch can still include a connector bar or plate that partially covers the roof of your mouth, dulling sensation to varying degrees.
Neurological Feedback: Why You Might Bite Your Cheek with Dentures
Your natural teeth aren't just for chewing — they're sensors. The periodontal ligament (PDL) surrounding each root sends continuous signals to your brain about bite force, pressure, and food texture. This is called proprioception, and it's what allows you to bite down on a grape without crushing it.
Dentures eliminate this feedback loop entirely. Because a denture "floats" on soft tissue, your jaw muscles lose the fine-tuned pressure data they're used to receiving. New denture wearers frequently report accidentally biting their cheeks or tongue — not due to poor fit, but because the brain is recalibrating without its usual sensory input.
Dental implants, fused directly to the jawbone, provide what researchers call "osseoperception" — a different but more reliable form of bite feedback transmitted through bone rather than a ligament. It's not identical to natural tooth proprioception, but it's far superior to nothing. According to the American Academy of Periodontology, full-mouth implants allow patients to bite and chew more naturally than conventional dentures — and this neurological connection is a significant reason why.
Implant-supported snap-in dentures offer a meaningful compromise. They anchor to two to four implants per arch, which stabilizes the prosthetic and partially restores the solid feedback your jaw muscles expect. A Healthline overview of snap-in dentures confirms that implant-retained options reduce gum friction and improve chewing control compared to conventional removable dentures.
When Your Health History — Not Your Budget — Chooses for You
I see patients who come in certain they want implants, and after reviewing their medical history, we have a different conversation. This is the part that online cost comparisons consistently skip.
Bisphosphonates and MRONJ risk. Patients taking bisphosphonate medications — Fosamax, Boniva, Reclast — for osteoporosis face a serious implant complication risk called Medication-Related Osteonecrosis of the Jaw (MRONJ). These drugs suppress bone turnover, which is exactly the process that allows an implant to osseointegrate. Implant failure rates rise, and in some cases, bone can die at the surgical site. If you've been on these medications for more than three years, implants may not be advisable at all.
Uncontrolled Type 2 diabetes. Elevated blood glucose impairs healing and increases infection risk post-surgery. Mayo Clinic lists systemic conditions that affect bone healing as direct contraindications for implant surgery.
Active smoking. Heavy smoking restricts blood flow to the gums and bone, significantly increasing implant failure rates. Research published in PMC confirms that smoking status is among the most impactful variables in long-term implant survival outcomes.
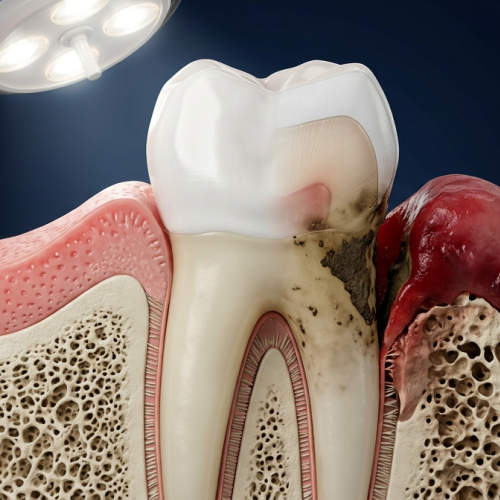
Insufficient bone density. Implants require enough jawbone volume to anchor the titanium post securely. Patients who've worn conventional dentures for years often experience significant bone resorption — the very problem that makes their dentures loose. In these cases, a bone graft may be needed before implants become viable, adding months and cost to the process.
For patients in any of these categories, removable partial dentures or implant-retained overdentures (which require fewer implants and less bone volume) often represent the more realistic and safer path. Patients dealing with gum disease or gingivitis should also have those conditions addressed before pursuing any tooth replacement option.
The Long-Term Math: Durability, Bone Loss, and Real Cost
Conventional dentures typically last seven to ten years with proper care before relining or replacement is needed. That sounds reasonable until you factor in what's happening underneath them. Without tooth roots stimulating the jawbone, bone resorption continues steadily — reshaping your face, altering your bite, and eventually making your dentures fit worse over time.
Dental implants interrupt that cycle. The titanium post acts as a functional root, preserving bone density and facial structure. Survival data is strong: a Healthline breakdown of implant benefits cites survival rates of 96.8% at ten years and 94% at fifteen years.
From a cost-effectiveness standpoint, implants carry a higher upfront investment but often prove more economical over a fifteen to twenty year horizon. Dentures require periodic relining, replacement, and adhesives. Implants, maintained like natural teeth, can last decades without replacement. Keeping up with routine cleaning and exam appointments is essential to maximizing the lifespan of any tooth replacement option.
Partial dentures — the option for patients missing several but not all teeth — fall somewhere between. Metal-framed partials can last five or more years, but clasps can stress adjacent natural teeth and accelerate their deterioration over time.
The honest answer to "which is better" is that implants outperform dentures biologically in almost every measurable way. But biology isn't the only variable. Candidacy, budget, and timeline are real constraints, and a removable option — done well — is far better than leaving a gap untreated. In some cases, a tooth crown may also be part of the broader restorative plan, depending on the condition of remaining teeth.
Ready to Find Out Which Option Fits Your Situation?
At Long Beach Family Dentist, we take a thorough look at your bone density, health history, and goals before recommending any tooth replacement option. Our Long Beach team handles everything from removable partial dentures to full-arch implant restorations — including advanced sedation for patients who are anxious about surgery. Schedule a consultation and get a clear, honest picture of what's actually right for you.
This article is intended for general informational purposes only and does not constitute professional dental or medical advice. Always consult a licensed dental professional for diagnosis and personalized treatment recommendations.